Luxury Recovery Centers USA: The 2026 Definitive Reference
The intersection of clinical necessity and high-end residential hospitality has created a sophisticated niche in the American healthcare landscape. In 2026, the term “recovery” has expanded beyond its traditional associations with substance use, now encompassing post-surgical rehabilitation, burnout-induced neurological recalibration, and executive mental health stabilization. For the discerning individual, the primary challenge is distinguishing between a “resort with clinical dressing” and a legitimate medical institution that uses luxury to facilitate healing.
Institutional recovery often fails because of the “Environmental Stress” inherent in traditional hospital settings. Sterile lighting, persistent auditory interruptions, and the lack of privacy can elevate cortisol levels, thereby inhibiting the body’s endogenous repair mechanisms. High-end facilities address this by engineering an environment that promotes parasympathetic nervous system dominance. When the nervous system exists in a “fight or flight” state, the efficacy of therapeutic and pharmacological interventions increases exponentially.
Understanding this sector requires an analytical look at the “Value of Privacy” and the “Cost of Anonymity.” For high-profile figures, the risk of a breach in confidentiality is a significant barrier to seeking care. High-end centers neutralize this risk through “Administrative Segregation” and rigorous digital security protocols. This editorial reference provides a definitive framework for evaluating these facilities, ensuring that the choice of a recovery center is grounded in institutional integrity and clinical rigor rather than mere aesthetic appeal.
Understanding “luxury recovery centers usa”

To master the selection of luxury recovery centers USA is to solve for “Clinical Coherence.” In a professional medical context, luxury is not an indulgence but a “Compliance Tool.” If a patient is comfortable, they stay longer; if they stay longer, the probability of a durable recovery outcome increases. However, the market is saturated with facilities that prioritize “Amenity Padding” over “Evidence-Based Protocol.”
Multi-Perspective Explanation
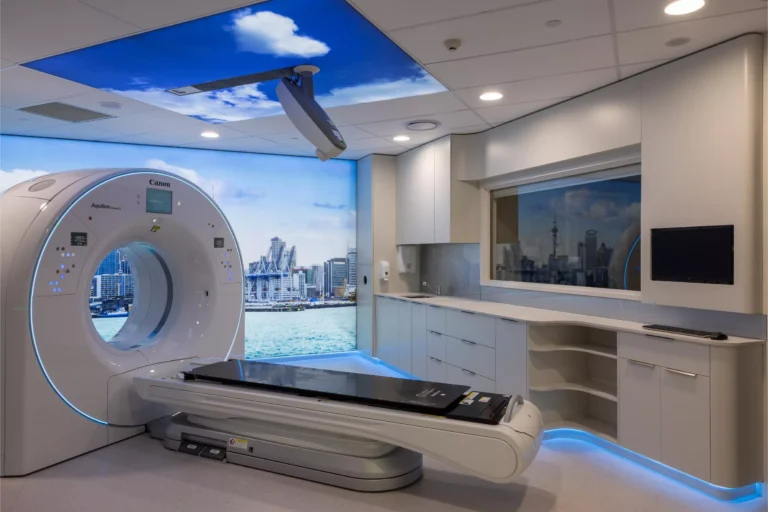
From a Neurobiological Perspective, luxury environments leverage “Biophilic Design” to reduce systemic inflammation. Features such as ocean views, natural wood textures, and circadian-aligned lighting are not just for show; they are environmental cues that signal safety to the amygdala. From a Logistical Perspective, these centers offer “Low-Ratio Care,” often providing a 3-to-1 or even 1-to-1 staff-to-patient ratio. This ensures that every nuance of a patient’s recovery from medication side effects to nutritional needs is monitored in real-time. From a Reputational Perspective, luxury recovery serves as a “Corporate Continuity” asset, allowing executives to recover in an environment where they can safely manage limited professional obligations without compromising their health.
Oversimplification Risks
The primary risk is “The Gilded Cage Fallacy,” the assumption that a high price tag guarantees a superior medical outcome. In 2026, many non-accredited facilities use high-end finishes to mask a lack of board-certified medical staff. A professional evaluation ignores the thread count of the linens and focuses instead on the “Credential Density” of the treatment team. True recovery excellence requires the seamless integration of hospitality and hematology.
Contextual Background: The Evolution of High-Acuity Hospitality
The American recovery industry has moved from the “Sanatorium” model of the early 20th century to the “Institutional Rehab” of the 1980s, and finally to the “Integrated Wellness Hub” of 2026. Historically, recovery was punitive or at least intentionally sparse. The shift toward luxury began when clinicians realized that “Stress is the Enemy of Sobriety and Healing.”
This evolution has led to the “Specialization of Space.” We no longer see one-size-fits-all centers. Instead, the market has bifurcated into ultra-niche facilities: some focusing exclusively on “Orthopedic Post-Op” for athletes, others on “Burnout Syndrome” for Silicon Valley engineers, and others on “Dual Diagnosis” for high-net-worth individuals. In 2026, the hallmark of a top-tier center is its “Interdisciplinary Depth”—the ability to have a psychiatrist, a physical therapist, and a nutritionist collaborate on a single patient’s daily itinerary.
Conceptual Frameworks for Therapeutic Immersion
Strategic recovery seekers utilize specific mental models to detect points of “Clinical Integrity” before committing to a stay.
1. The “Continuum of Care” Framework
This model posits that recovery is a three-phase process: Stabilization, Integration, and Maintenance. A luxury center that only focuses on the “In-patient” phase without providing a “Sober Living” or “Out-patient” bridge is functionally incomplete. This framework dictates that the “Best” center is the one that manages the patient’s re-entry into their high-pressure life.
2. The “Holistic-Clinical Hybrid” Logic
High-end centers often blend “Eastern” modalities (meditation, acupuncture) with “Western” medicine (pharmacotherapy, neurofeedback). This framework evaluates a center based on its “Evidence Threshold.” If the facility cannot explain the clinical mechanism behind their “Equine Therapy” or “Sound Bath,” they are likely utilizing “Placeholder Therapies” to fill the schedule.
3. The “Privacy-to-Protocol” Ratio
For many in this demographic, privacy is a medical necessity. If a patient is anxious about being seen, their sympathetic nervous system remains active. This framework analyzes a center’s “Physical Security” and “Digital Anonymity” as clinical interventions. A center with a private entrance and a non-disclosure agreement (NDA) for all staff members is often more effective than a higher-rated medical facility with a public lobby.
Key Categories of Recovery Specialization
Selecting the right facility involves recognizing the “Primary Impediment” to the patient’s health.
| Category | Primary Focus | Staffing Profile | Trade-off |
| Medical Detox | Physiological stabilization. | MDs, Nurses, Toxicologists. | Highly clinical; less “resort” feel. |
| Executive Burnout | Cortisol/Adrenal regulation. | Psychologists, Sleep Coaches. | Can feel like a “Work-Cation.” |
| Post-Surgical | Orthopedic/Tissue healing. | PTs, OTs, Wound Care. | Requires proximity to a hospital. |
| Dual Diagnosis | Mental Health + Substance. | Dual-certified Clinicians. | Longer duration; high intensity. |
| Trauma/PTSD | Neurological recalibration. | Trauma Specialists, EMDR. | Intense psychological demand. |
| Nutritional/Metabolic | Gut-Brain Axis. | RDNS, Functional Medicine. | Strict dietary restrictions. |
Detailed Real-World Scenarios and Decision Logic
The “High-Functioning” Alcoholism Case
A CEO needs treatment, but cannot disappear for 30 days without causing a shareholder panic.
-
The Red Flag: A center that bans all electronic devices.
-
The Decision Logic: Selection of a center with “Executive Suites” that allows for “Structured Work Windows.”
-
Outcome: The CEO stabilizes their health while maintaining corporate “Pulse Checks,” preventing a secondary crisis at work that would have triggered a relapse upon return.
The Post-Orthopedic Complication
A professional athlete undergoes a complex knee reconstruction and needs “High-Frequency” physical therapy.
-
The Decision Logic: Selection of a center that houses its own MRI and “Anti-Gravity Treadmills.”
-
Failure Mode: Choosing a center based on the quality of its “Organic Menu” while neglecting its “Rehab Hardware.”
-
Outcome: The athlete receives four hours of PT daily, compared to the one hour typical of home-based recovery, accelerating their return-to-play timeline by 20%.
Planning, Cost, and Resource Dynamics
The “Cost” of luxury recovery is a factor of “Personnel Density” and “Environmental Exclusivity.”
Budgetary Impact of Luxury vs. Standard Recovery (2026 Estimates)
| Feature | Luxury Recovery Center | Standard Center | The “Difference” Driver |
| Weekly Rate | $15,000 – $60,000 | $3,000 – $7,000 | Exclusivity and Staff Ratios. |
| Staff Ratio | 1:1 to 3:1 | 10:1 to 15:1 | Personalized “Vigilance.” |
| Dining | Private Chef (Nutrigenomics) | Cafeteria/Catering | Therapeutic nutrition. |
| Room | Private Suite/Villa | Shared/Semi-Private | Psychological safety/Privacy. |
| Aftercare | 12-month Concierge | 30-day Referral | Preventing “Relapse Drift.” |
Tools, Strategies, and Support Systems
A definitive strategy for navigating luxury recovery centers USA involves a “Validation Stack”:
-
The CARF/Joint Commission Audit: Never consider a facility that does not hold current accreditation from the Commission on Accreditation of Rehabilitation Facilities (CARF) or The Joint Commission.
-
The “Bio-Marker” Integration: Top centers in 2026 use “Continuous Glucose Monitors” (CGM) and “HRV Wearables” to adjust a patient’s program daily.
-
The “Shadow Staff” Inquiry: Ask if the center uses “Agency Staff” or “Contractors.” High-end centers should have a 90%+ permanent employee rate to ensure continuity of care.
-
Pharmaceutical Transparency: Request a copy of the “Formulary.” A facility that relies heavily on sedatives (the “Zombification” method) is often masking a lack of psychological support.
-
The “Exit-Entry” Protocol: Review the “Discharge Plan” on Day 1. If they don’t have a plan for your first 48 hours back home, the clinical strategy is shallow.
-
Alumni Network Strength: Ask to speak with an alumnus of the program. Legitimate centers have a network of former patients who can speak to the “Long-Term Efficacy.”
Risk Landscape and Failure Modes
The “Taxonomy of Risk” in high-end recovery includes:
-
The “Conduit” Failure: A facility where staff are easily bribed to bring in contraband or unauthorized visitors due to the patient’s wealth/status.
-
The “Clinical Hollow” Mode: A center that spends 80% of its budget on marketing and real estate and 20% on clinicians.
-
The “Isolation Paradox”: A patient becomes so comfortable in the luxury environment that they develop “Institutional Anxiety” about leaving, making reintegration impossible.
-
The “Privacy Breach” Risk: In the age of 2026 surveillance, centers with poor “Cyber-Hygiene” are vulnerable to digital leaks of patient records.
Governance, Maintenance, and Long-Term Adaptation
Recovery is not a “Reset”; it is a “Reprogramming.”
-
The “Bi-Weekly Review”: In a high-end center, the treatment plan should be “Dynamic,” not “Static.” If the plan hasn’t changed in 14 days, the staff is likely coasting.
-
The “Transition Buffer”: The most successful patients spend their last 7 days in a “Step-Down” villa where they manage their own time and meals before leaving.
-
Layered Checklist for Clinical Vetting:
-
Is the Medical Director board-certified in Addiction or Physical Medicine?
-
Does the center have a formal partnership with a nearby Level 1 Trauma Center?
-
Are all therapists licensed at the Master’s level or higher?
-
Can the facility accommodate specific “Religious” or “Ethical” dietary requirements?
-
Is there a dedicated “Family Liaison” to handle the patient’s domestic dynamics?
-
Measurement, Tracking, and Evaluation Signals
How do you measure the “Success” of a $100,000 stay?
-
Leading Indicators: Sustained improvement in “Sleep Architecture” and “Heart Rate Variability”; the patient’s ability to articulate a “Coping Strategy” for their specific triggers.
-
Qualitative Signals: The “Staff Retention” rate. High turnover in staff almost always correlates with poor patient outcomes.
-
Documentation Examples: The “Bio-Psychosocial Assessment”—a comprehensive 20-page document produced at intake that serves as the baseline for all future progress.
Common Misconceptions and Oversimplifications
-
“Luxury Makes it Easier”: Luxury makes it tolerable, but the psychological work remains difficult. A massage is not a substitute for a trauma session.
-
“I Only Need 28 Days”: The “28-day” model is based on 1950s insurance cycles, not modern neuroscience. Many high-end centers now recommend 60–90 days for neurological stabilization.
-
“Private Chefs are for Pleasure”: In 2026, “Nutritional Psychiatry” is a core clinical pillar. Food is used to repair the gut-brain axis, which is often damaged by stress or substances.
-
“Celebrity Centers are the Best”: Fame is a marketing metric, not a clinical one. Centers that cater to “Influencers” often have the highest relapse rates.
-
“Insurance Won’t Cover Luxury”: While insurance rarely covers the “Room and Board” of a villa, they often cover the “Clinical Minutes” of the MDs and therapists.
-
“I Can Work While I Recover”: While “Pulse Checks” are okay, “Business as Usual” prevents the brain from entering the “Theta State” required for deep healing.
Ethical and Practical Considerations
In 2026, the ethics of luxury recovery centers USA revolve around “Clinical Honesty.” Is the center telling the patient what they want to hear or what they need to hear? A center that acts as a “Yes-Man” to a wealthy patient is ethically bankrupt. Practically, the patient must consider the “Transferability of the Environment.” If you can only be healthy while staring at the Pacific Ocean, the treatment has failed to provide you with the tools to be healthy in a boardroom in New York.
Conclusion
The architecture of a durable recovery is built on “Intentional Design.” By mastering the selection of a luxury center, the patient transitions from being a “Recipient of Care” to a “Sovereign of their Health.” Success is found in the “Quiet Resilience,” the ability to return to a high-pressure life with a nervous system that is no longer reactive, but responsive. In 2026, the most effective recovery centers are those that realize that while the view from the window is beautiful, the work done inside the room is what saves the life.