Compare Bariatric Surgery Plans: The Definitive 2026 Editorial Guide
The clinical management of severe obesity has transitioned from a niche surgical intervention to a comprehensive metabolic discipline. For the serious patient or healthcare strategist, bariatric surgery is no longer viewed as a singular event but as a sophisticated, lifelong physiological recalibration. Navigating the modern landscape of surgical weight loss requires an analytical departure from surface-level brochures in favor of a deep, systemic understanding of how restrictive and malabsorptive mechanisms interact with human endocrinology.
In 2026, the divergence between “volume-based” surgical centers and “precision metabolic” programs has never been more pronounced. Identifying the optimal path involves a synthesis of surgical physics, nutritional biochemistry, and financial engineering. A premier plan is an ecosystem one that accounts for the patient’s baseline metabolic rate, hormonal signaling (such as GLP-1 and ghrelin), and the long-term structural integrity of the gastrointestinal tract.
To engage with this sector as an informed participant is to acknowledge that surgery is a tool of “Metabolic Leverage.” This leverage is only effective when the underlying clinical roadmap is resilient enough to accommodate the complexities of “weight-loss plateaus,” micronutrient absorption variables, and the psychological shifts that accompany massive physiological change. This editorial reference provides a definitive exploration of the current restorative landscape, prioritizing technical nuance and clinical honesty.
Understanding “compare bariatric surgery plans.”
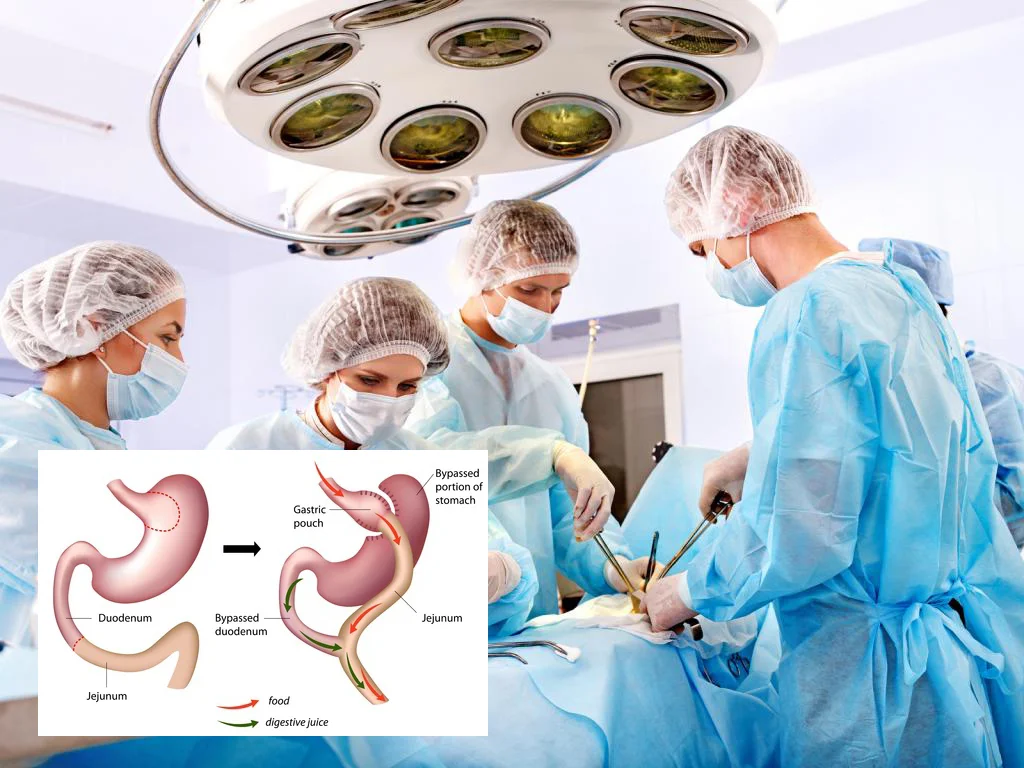
To effectively compare bariatric surgery plans, one must first decouple the surgical procedure from the broader clinical “plan.” In a professional medical context, a plan is a longitudinal strategy that begins months before the first incision and extends decades beyond it. It encompasses the surgical technique, the perioperative nutritional protocol, the behavioral health integration, and the financial structure (insurance versus self-pay logistics).
Multi-Perspective Explanation
-
The Metabolic Perspective: From this viewpoint, a plan is judged by its ability to resolve comorbidities such as Type 2 Diabetes or Sleep Apnea. A “top” plan is one that prioritizes hormonal signaling changes over simple caloric restriction.
-
The Structural Perspective: This focuses on the permanent alteration of the anatomy. A plan must account for the “Serviceability” of the revision if a patient gains weight back ten years later. Does the plan leave room for secondary surgical adjustments?
-
The Logistical Perspective: Evaluation is based on the “Support Tether.” A premier plan includes a dedicated “Bariatric Navigator” and life-long access to specialized bariatric dietitians who understand the unique absorption profiles of a bypassed stomach.
Oversimplification Risks
The most significant risk in current bariatric planning is “Procedure Bias”—the belief that the surgery itself does the work. An oversimplified view often suggests that a “Sleeve” is better than a “Bypass” simply because it is faster to perform. This ignores the biological reality of acid reflux or sweet-eating habits, which can render a sleeve ineffective while a bypass might succeed. A professional assessment avoids these oversimplifications by analyzing the patient as a complex bio-mechanical system.
Contextual Background: The Evolution of Metabolic Surgery
The history of weight-loss surgery has evolved from “Jejunoileal Bypass” (JIB) in the 1950s, which caused extreme malabsorption and liver failure,e to the “Precision Era” of 2026. Early bariatric interventions were “blunt instruments” designed solely to prevent the body from absorbing food. They were plagued by high complication rates and a lack of understanding of the “Incretin Effect.”
By the early 2010s, the laparoscopic revolution made these surgeries safer and more accessible. Today, in 2026, the evolution is driven by the integration of robotics and “Pharmacotherapy Synergies.” Modern plans often utilize a “Hybrid Model,” where surgery provides the structural baseline and GLP-1 medications are used to manage “Breakthrough Hunger” during the maintenance phase. We are no longer just “shrinking stomachs”; we are re-engineering the chemical conversation between the gut and the brain.
Conceptual Frameworks and Mental Models for Evaluation
Veterans of the bariatric field utilize specific frameworks to evaluate the viability of a plan for a specific patient.
1. The Restriction-to-Malabsorption (RtM) Ratio
This model evaluates the mechanism of the plan. A “Sleeve Gastrectomy” is 100% restrictive (smaller pouch), while a “Biliopancreatic Diversion” is high-malabsorptive. A plan must align this ratio with the patient’s eating behavior. A “snacker” or “grazer” will fail a purely restrictive plan; they require a malabsorptive component to mitigate the constant intake of small calories.
2. The “Biological Set-Point” Framework
This posits that the body has a defended weight level. Surgery is the only intervention capable of lowering this set-point by altering hormones like PYY and Ghrelin. The FTP (Failure to Progress) model helps a clinician identify if a plan is aggressive enough to overcome the patient’s specific hormonal resistance.
3. The “Lifelong Serviceability” Model
As the body ages, the surgical site changes. This model favors procedures that allow for “Endoscopic Surveillance.” For example, a Sleeve allows for easy access to the duodenum for future gallbladder or bile duct issues, whereas a traditional Bypass creates a “Blind Limb” that is harder to reach with standard medical tools.
Key Categories and Physiological Variations
The surgical landscape is categorized into distinct “Operational Profiles,” each with its own mechanical trade-offs.
| Profile | Mechanism | Primary Benefit | Significant Constraint |
| Gastric Sleeve (LSG) | Restrictive | Lower risk of vitamin deficiency; no “dumping.” | Can worsen chronic acid reflux (GERD). |
| Roux-en-Y (RYGB) | Hybrid | “Gold Standard” for diabetes resolution. | Risk of internal hernias and marginal ulcers. |
| Duodenal Switch (DS) | Malabsorptive | The highest percentage of weight loss. | Requires 80g+ protein daily; frequent bowel movements. |
| SADI-S | Hybrid | Modernized DS; fewer bowel complications. | Newer procedure; fewer long-term (20-year) data points. |
| Gastric Balloon | Temporary | Non-surgical; no permanent changes. | Must be removed in 6 months; lower total weight loss. |
Realistic Decision Logic
The selection of a profile must be driven by the Patient’s Comorbidity Profile. A patient with severe, medicated GERD (acid reflux) should rarely be placed in a “Sleeve” plan, as the surgery creates a high-pressure system that will exacerbate the reflux. For this patient, a “Bypass” is the logical choice, as it is a low-pressure system that effectively cures reflux while providing weight loss.
Detailed Real-World Scenarios and Decision Logic

The “Sweet Eater” with Type 2 Diabetes
A patient has a BMI of 45 and a significant habit of consuming liquid sugars.
-
Decision Point: Sleeve vs. Bypass.
-
Analysis: The “Dumping Syndrome” associated with a Bypass acts as a “Negative Feedback Loop” (nausea/sweating) when sugar is consumed. This behavioral deterrent is absent in a Sleeve.
-
Outcome: The Bypass provides the hormonal “incretin” boost to resolve the diabetes, while the dumping syndrome manages the sweet-eating behavior.
The “Extreme Athlete” with Obesity
A patient with a BMI of 40 who is highly active but cannot lose weight due to excessive hunger.
-
Constraint: Requires high energy for performance; cannot afford severe malabsorption of minerals.
-
Decision Point: Sleeve Gastrectomy.
-
Second-Order Effect: The Sleeve preserves the intestinal path, allowing for standard absorption of performance-critical electrolytes and iron, while reducing the stomach capacity to manageable levels.
Planning, Cost, and Resource Dynamics
The financial dynamics of bariatrics are influenced by “Insurance Payer Requirements” and the “Cost of Complications.”
Range-Based Operational Cost Table (US Estimates 2026)
| Cost Component | Insurance (Typical Co-pay) | Self-Pay Range | Variability Factors |
| Pre-Op Clearance | $500 – $1,500 | $2,000 – $4,000 | Psych/Cardiac/Sleep clearances. |
| Surgical Hospital Fee | $1,000 – $5,000 | $12,000 – $25,000 | Robot-assisted vs. Traditional Lap. |
| Surgeon & Anesthesia | $500 – $2,500 | $4,000 – $8,000 | Surgeon’s volume and experience. |
| Long-Term Supplements | $50 – $100 / month | $50 – $100 / month | Bariatric-specific multi-vitamins. |
Note: Opportunity cost is critical. A “Budget” plan in a different country might save $10,000 initiall,y but results in a “Logistical Desert” when a complication occurs. Professional plans prioritize local follow-up care as the primary insurance against long-term failure.
Support Systems, Tools, and Strategic Resources
A successful metabolic reconstruction relies on a “Support Stack” of specialized resources:
-
Impedance Scales: To track muscle mass preservation versus fat loss.
-
Bariatric-Specific Micronutrient Panels: Blood tests that look for obscure deficiencies like Copper or Selenium, which are often missed in standard physicals.
-
Support Groups (Digital & Local): To manage the “Social Friction” that occurs when a patient’s personality and appearance change rapidly.
-
Endoscopic Suturing: A tool for “Pouch Tightening” if the original surgery stretches over time.
-
Smart Food Journals: Utilizing “Visual Recognition” to track protein-to-carb ratios accurately.
-
Bone Density Scans (DEXA): To monitor for calcium depletion, a common risk in malabsorptive plans.
Risk Landscape and Failure Modes
Even the most prestigious bariatric plans harbor compounding risks.
-
The “Transfer Addiction” Trap: When the “food addiction” is resolved, patients are at a higher risk for alcoholism or gambling, as the brain seeks a new dopamine source.
-
Marginal Ulcers: Primarily in Bypass plans, these occur at the connection point between the stomach and intestine, often triggered by NSAIDs (aspirin/ibuprofen) or smoking.
-
Nutritional “Washout”: In high-malabsorptive plans, a simple stomach flu can lead to rapid dehydration and critical vitamin depletion requiring IV intervention.
Governance, Maintenance, and Long-Term Adaptation
To maintain the quality of a bariatric outcome, patients must adopt a “Governance” mindset.
-
The Annual “Metabolic Audit”: A full panel of bariatric bloodwork every 12 months for life.
-
Protein-First Protocol: A governance rule where every meal begins with 20-30g of dense protein to protect muscle mass.
-
Adjustment Triggers: If a patient regains 10% of their lowest weight, the plan must pivot to an immediate “Reset” which may include pharmacotherapy or a nutritional intensive.
Measurement, Tracking, and Evaluation Signals
How do you measure the success of a bariatric plan?
-
Leading Indicators: Percentage of Excess Weight Loss (%EWL); resolution of blood pressure medications; return of mobility.
-
Qualitative Signals: The “Non-Scale Victory” (NSV)—fitting into a standard airplane seat or playing with grandchildren without fatigue.
-
Documentation: Maintaining a “Surgical Record” that includes the exact length of the intestinal bypass limbs, as this determines the severity of malabsorption.
Common Misconceptions and Oversimplifications
-
“It’s the Easy Way Out”: Surgery is a “Power Tool” that requires significant psychological and physical labor to use correctly.
-
“The Stomach Stretches Back”: While the pouch can expand slightly, “failure” is usually due to the brain finding “Slider Foods” (chips/ice cream) that bypass the feeling of fullness.
-
“You Can Never Eat Normal Again”: Within 12-18 months, most patients eat standard foods, just in significantly smaller, “quality-over-quantity” portions.
-
“Weight Regain is Inevitable”: Long-term studies show that 70-80% of patients maintain significant weight loss at the 10-year mark when following a structured plan.
-
“It’s Only for the Morbidly Obese”: In 2026, many plans start at a BMI of 30 if the patient has metabolic syndrome.
-
“The Cheapest Surgery is the Best Value”: Value in bariatrics is measured by “Complication-Free Years,” not the initial invoice.
Ethical and Practical Considerations
As surgical bariatrics becomes more common, the “Ethical License” of the provider is critical. This means refusing surgery to patients with untreated eating disorders or those seeking “aesthetic” weight loss without metabolic need. A premier plan operates with intellectual honesty, acknowledging that surgery is a life-altering trade-off—exchanging the risks of obesity for the risks of a modified anatomy.
Conclusion
The architecture of a healthier metabolic future is a strategic exercise in aligning medical engineering with human biology. It is a transition from being a victim of one’s genetics to being an active governor of one’s physiology. Whether you are considering a Bypass, a Sleeve, or an SADI-S, success depends on the alignment of technical precision, anatomical respect, and lifelong maintenance. In 2026, the ultimate luxury in bariatric medicine is not the weight loss itself, but the metabolic freedom—the ability to live a life no longer dictated by the hormonal signals of hunger and the structural burdens of excess weight.